ABO incompatibility is a common and generally mild type of haemolytic disease in babies. The term haemolytic disease means that red blood cells are broken down more quickly than usual. Due to the increased breakdown of red blood cells, jaundice, anaemia, and in very severe cases can cause death, can result. During pregnancy ABO incompatibility may occur if:
1. The mother and baby’s blood types are incompatible
2. Different blood types come into direct contact with each other and,
3. Antibodies form
Significant problems with ABO incompatibility occur mostly with babies whose mothers have the O blood type and where the baby is either A or B blood type. Premature babies are much more likely to experience significant problems from ABO incompatibility. Conversely, healthy full-term babies are generally only mildly affected. Unlike haemolytic disease that can result in the birth of a second baby when a mother has a negative blood group, ABO incompatibility can occur in first-born babies. Additionally, it does not become more severe in future pregnancies.
Understanding ABO Incompatibility
When understanding ABO incompatibility, it is helpful to review the different blood groups. The genes you inherit from your parents determine your blood group. There are four blood types; A, B, AB and O. Each blood type has its collection of chemicals on the blood cell surface known as antigens. To clarify, type A has the A antigen, B has the B antigen, AB has both antigens and O contains no antigen. Therefore if different blood types mix, an immune response occurs. As a result, the person may produce antibodies to attack the foreign blood antigen.

During pregnancy, the mother’s and baby’s blood generally do not mix. It’s important to realise that the mothers and babies circulation is kept separate by the placental membrane. Though oxygen, carbon dioxide, nutrients, certain drugs and some viruses can pass through the placental membrane. Furthermore, some circumstances may cause the two blood types to mix. Examples of events increasing the risk of the two blood types mixing include miscarriage, trauma and a babies birth. Surprisingly two blood types may mix for reasons unknown.
Antibody Formation
Antibodies form against foreign blood types such as type A and B. These antibodies could then pass across the placental membrane and enter the baby’s circulation. Antibodies can destroy some of the baby’s red blood cells. This destruction of red cells causes an increase in the production of bilirubin – a waste product. If the baby’s body produces too much bilirubin, it can overwhelm the baby’s normal waste elimination processes and lead to jaundice.
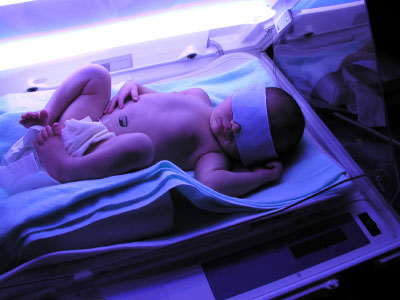
An increase in bilirubin causes jaundice, a pigment that turns the newborn’s skin yellow. Additionally, jaundice can cause the whites of the baby’s eyes to have a yellow appearance. During an examination, your midwife or doctors observers the colour of your baby’s skin. If your baby looks yellow, performing a blood test can confirm the level of jaundice. Slight jaundice is very common in newborns and requires no follow-up. Babies with high levels of bilirubin in their blood will require phototherapy. Furthermore, severe cases of jaundice may need an exchange blood transfusion.
Anaemia in Babies
For babies effected by ABO incompatibility, anaemia may become an issue after a few weeks. The anaemia is caused by the faster than usual breakdown of the baby’s red blood cells caused by the mother’s antibodies. These antibodies can linger in the baby’s circulation for weeks after birth. Because of this, some babies will need to have blood tests to check the level of anaemia.
Routine Blood Testing
Routine blood screening tests in pregnancy doesn’t screen for ABO incompatibility. Furthermore, testing in pregnancy does not improve outcomes for the baby. Unfortunately, there are no preventative measures for ABO incompatibility.
After birth, there are two options for testing for ABO incompatibility:
- Have the cord blood of all babies whose mothers have an O blood group and the father either type A or B blood tested. The theory behind this approach is that if the baby is either type A or B, and, they test positive for direct antiglobulin tests (DAT), the baby can then be followed closely for jaundice.
- The alternate approach is to screen any baby who becomes significantly jaundiced (particularly within the first 24 hours).


Hi Jane , thank you for your article. I have had 3 pregnancies , first was a miscarriage at 12weeks, second was successful full term but emergency c-section due to abrupted placenta and third was another successful pregnancy with elective c-section at 37weeks due to antibodies.
My question is have you worked with pregnant mothers with antibodies that were able to plan for a VBAC ? I can only imagine a low dose TO INDUCE would BE administered to have baby at 37weeks…?? A guess.
Planning for another child , I am trying to work our all my options, as recent blood tests show the previous antibodies are still present.
Thanks you for your time.
Hi Nina – it is wonderful that you are exploring your options. There are a number of different types of antibodies and their impact on pregnancy and/or baby vary. Your comment doesn’t mention which type of antibodies. Have you considered consulting a midwife or doctor who is supportive of VBAC while you are considering another pregnancy? They can look back at your previous pregnancies and explore options open to you. Good luck in your search for information.
I just lost a baby due to ABO incompatibility at 34 weeks. I’m type O the baby was type A. I am only 22 y/o and extremely worried I won’t be able to have other successful pregnancies due to the same issue.
Hi Sarah – I am so sorry to hear of your loss. Have you spoken to an obstetrician about future pregnancies? Getting as much information as possible may help.
hi jane, my firstborn had jaundice within the first 24hrs after birth, he was on phototherapy for a week and got discharged. second born also had jaundice within the first 24hrs after birth, and died at day four of life. my question is, could my babies be suffering from ABO incompatibility because am blood group O and the dad is blood group B?
Hi Njeri – I am really sorry for the loss of your baby. Did the doctors give you a diagnosis or a reason for your baby’s jaundice? They usually do lots of tests and tell parents what type of jaundice their baby has.
Though have been taught since 1980’s that – in ABO incompatibility, the first born child is most likely to manifest sx’s & signs including change in red cells, high bilirubin, etc yet I have never found the likely mechanism for the traditionally understood observation of first born kids most frequently manifest even while overall incidence is low. I also know that recurrence in siblings with same ABO
HAVE >80% risk as well.
As an 0+ mom my own first child had severe reaction in spite of phototherapy developed sx’s & signs of kernicterus w/ low tone, altered reflexes, increased irritability, a strange high pitch cry, altered RBC’s & a bili level over 24. Though exchange began preparations he got better in time to avoid My next 4 A+ kids had no such difficulties and most had only mildest bili elevation. All 5 kids had same homozygous A+ dad. Again, I am aware the first born is not a fast rule as have seen babies who are 2nd, or 3rd etc be the child most impacted.
This site is so very kind and generous. Over the years I have seen endless reviews noting: “ABO HDFN is more common than Rh HDFN and may occur during the first pregnancy.” But then no article goes on to discuss or theorize why this is often true. Would appreciate even a link or reference I can read. I work in medicine & decades have not given me reasons why/ though RH-Neg pregnancies may have worse untreated outcome w/ each subsequent newborn yet ABO tends to go the other way. And it has also been tough to know WHY certain ethnic groups manifest with > incidence & > severity than Caucasian births good luck also learning why, what’s the mechanism? In this later issue find only isolated reports such as “High incidence seen in Jamaican Newborns due to Gut Flora” Thanks a million; great site!